Acupuncture can provide constipation relief while maintaining a healthy pregnancy. A combination of San Jiao 6 (Zhi Gou) and Stomach 36 (Zu San Li) is excellent for treating constipation during pregnancy. San Jiao 6 is the shu-stream and fire point of the San Jiao channel. It can regulate the qi of the three jiaos, unblock the qi of the fu organs, descend counterflow fire, open the orifices, activate the collaterals to disperse stagnation, and eliminate distention to stop pain.
It’s Time to Stop Prescribing Points
- The term prescription smuggles in a pharmaceutical logic: find the right agent, deliver it and expect a result. Drug > Administration > Effect. When translated into needling, this becomes: Point > Insertion > Effect.
- A generation of graduates can recite point combinations with poetic precision but lack the tactile intelligence to respond when a patient’s body contradicts the textbook.
- If expertise is defined as memorizing lists, we can be replaced by an algorithm. But if expertise is defined as sensing, deciding, modulating, and confirming, the practitioner becomes irreplaceable.
In a quiet corner of a busy teaching clinic, a student stands over a patient, needle poised. They have a “perfect” prescription: a textbook combination of points harvested from a lecture slide on chronic lower back pain. But as the needle meets the skin, the student hesitates. The tissue is dense, resisting entry. The patient’s breath is shallow. The student looks at the chart, then at the point, waiting for a result that hasn’t arrived. They know the map perfectly, but they are lost in the landscape.
The Problem With Our Vocabulary
This hesitation is the symptom of a quiet habit that has taken hold of our profession. In our classrooms, treatment rooms and journals, we routinely say we “prescribe” points. It sounds efficient. It echoes the authority of biomedical culture and fits neatly into the insurance field. But vocabulary is never neutral; repeated long enough, it dictates behavior.
The term prescription smuggles in a pharmaceutical logic: find the right agent, deliver it and expect a result. Drug > Administration > Effect. When translated into needling, this becomes: Point > Insertion > Effect. The symmetry is elegant, but it is fundamentally false.
The Huangdi Neijing does not describe a world of automatic reactions.1 It describes a world of regulation, timing and response. It places the burden of efficacy on the practitioner’s capacity to recognize change and guide it. Without the engagement of qi, there is a position but no therapy. When we “prescribe,” the practitioner risks becoming a mere delivery mechanism. To reclaim our identity, we must shift toward a more faithful phrase: point selection strategy.
|
KEY TAKEAWAYS FOR THE CLINICIAN |
The Hidden Curriculum
Every training program runs two syllabi. One is printed in the handbook; the other is whispered in everyday speech. When learners constantly hear about “prescriptions,” they begin to believe that effects are inherent in the points themselves – that technique is decorative, and deqi is optional.
The result is a generation of graduates who can recite point combinations with poetic precision but lack the tactile intelligence to respond when a patient’s body contradicts the textbook. By shifting our language to strategy, the paradigm transforms. Points become portals rather than pills, and the practitioner becomes the instrument rather than the administrator. Competence moves from rote recall toward sensory perception.
A Point Is Not a Pill
A medication is designed for chemical stability; a needle is a tool of modulation. An acupuncture outcome varies wildly based on angle, depth, pacing, and the patient’s readiness. As Hugh MacPherson noted, tightly scripted protocols often fail to resemble the clinical reality where adaptation defines effectiveness.2
If the effect depends on the feedback loop between hand and tissue, the word prescription collapses a living exchange into a static list. Our resemblance to biomedicine might increase, but our clinical accuracy decreases.
Consider a chef. A recipe describes potential, but dinner only happens when the cook senses the heat and aroma and makes a real-time correction. Two people can follow the same instructions; one produces nourishment, the other produces mere compliance. The difference is judgment.
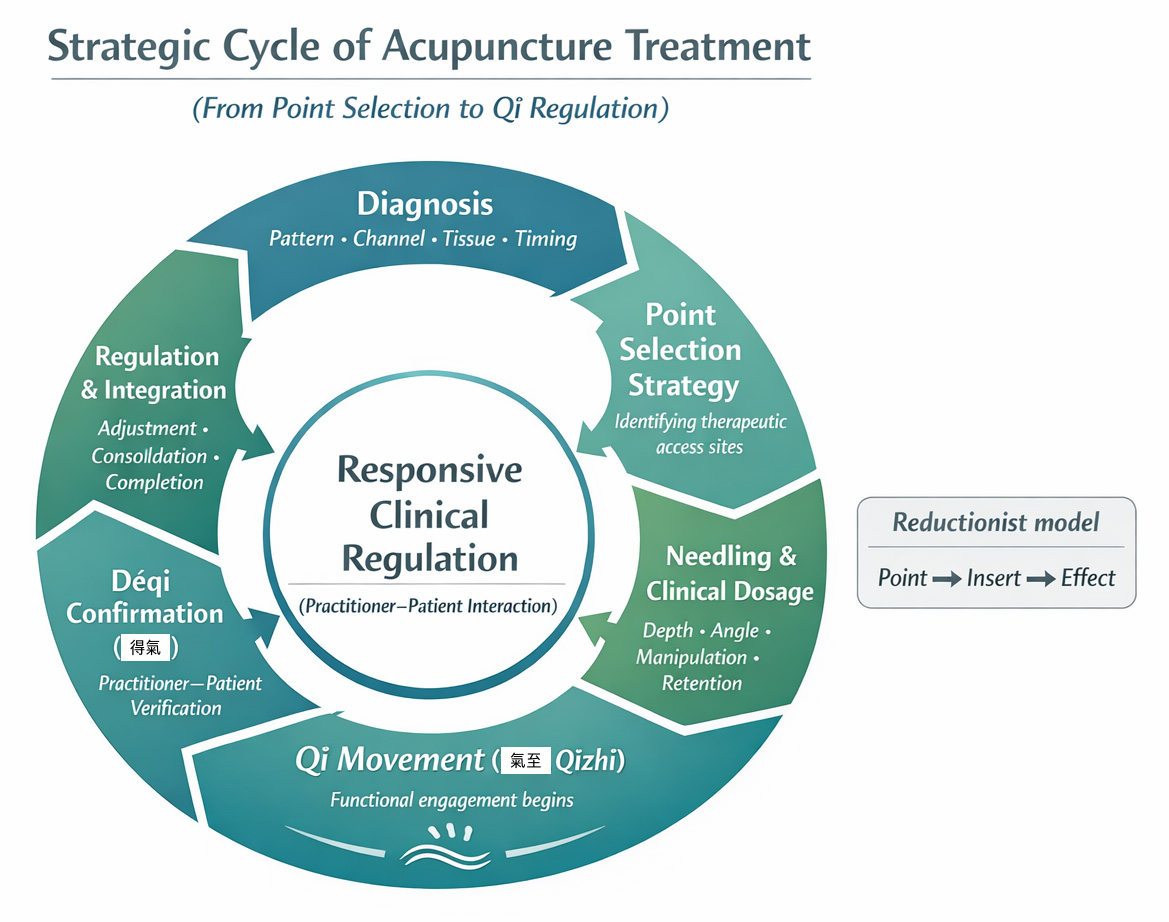
What “Strategy” Looks Like in Practice
A strategy-based approach recognizes that selection only prepares the field. The true arc of treatment looks like this:
- Diagnosis: Identifying the pattern
- Strategic Entry: Choosing the points
- Method and Modulation: The physical craft of needling
- Qi Movement (qizhi): The initiation of change
- Confirmation (deqi): The perception of engagement
- Regulation: Stabilizing the system
This sequence makes clinical reasoning visible. A chart note that simply lists “LI 4, LV 3” is just geography. A strategy-based note – “Distal-local regulation initiated; bilateral deqi obtained; myofascial guarding reduced” – is evidence of a thinking clinician.
The Stakes of Our Language
If expertise is defined as memorizing lists, we can be replaced by an algorithm. But if expertise is defined as sensing, deciding, modulating, and confirming, the practitioner becomes irreplaceable.
Invisible labor – the subtle adjustments we make at the needle head – is often undervalued labor. Precision in our language protects the value of what we actually do. It reminds the world that acupuncture is not just something we give; it is a craft we perform.
Where Change Begins
We do not need a reform committee to fix this. We simply need to ask better questions. In our clinics, let us stop asking “What is the point for X?” Instead, let us ask: “What is my intention? What movement is required? Where is access available right now?”
When our speech evolves, our training follows. When our training follows, our care deepens. It is time to stop prescribing points and start teaching a strategy. Because points open doors, but they do not walk through them.
References
- Unschuld PU. Nan Jing: The Classic of Difficult Issues, 2nd Edition. University of California Press, 2016.
- MacPherson H, Hammerschlag R. Acupuncture and the emerging evidence base: contrived controversy and rational debate. J Acupunct Meridian Stud, 2012 Aug;5(4):141-7.